Passive Euthanasia in India: Harish Rana Case | UPSC
Mar, 2026
•8 min read
Why in the News?
The Supreme Court of India, in the Harish Rana vs Union of India Case (2026), authorised passive euthanasia for 32-year-old Harish Rana, who has remained in a persistent vegetative state (PVS) for 13 years. The ruling marks the first real-world application of India’s passive euthanasia. The case has drawn attention to legal safeguards under Article 21 (Right to die with dignity).
Background of the Harish Rana Case
Harish Rana suffered severe head injuries after an accidental fall from balcony in 2013 and remained in a persistent vegetative state with complete quadriplegia for over 13 years. His father approached the Delhi High Court in 2024 seeking withdrawal of treatment, but the plea was rejected.
The family then moved the Supreme Court of India. A bench led by Justice J. B. Pardiwala and Justice K. V. Viswanathan set up two medical boards, which found recovery chances negligible. Based on this, the Court allowed withdrawal of life-sustaining treatment, marking the first real application of India’s passive euthanasia framework.
What is Euthanasia?
Euthanasia refers to the deliberate act of ending the life of a person suffering from an incurable disease or irreversible condition to relieve pain and suffering. It is typically carried out by a physician and is broadly classified into active and passive euthanasia.
| Active Euthanasia | Passive Euthanasia |
|---|---|
| Active euthanasia involves directly causing the death of a patient through deliberate medical intervention. | Passive euthanasia involves withdrawing or withholding life-sustaining medical treatment. |
| It is carried out by administering lethal injections or drugs by a doctor. | It is carried out by stopping ventilators, artificial nutrition, or other life-support systems. |
| In this case, death occurs due to a direct medical act. | In this case, death occurs naturally due to the underlying illness. |
| Active euthanasia is illegal in India under the Bharatiya Nyaya Sanhita and may amount to culpable homicide or abetment to suicide. | Passive euthanasia is legally permitted in India under safeguards laid down by the Supreme Court of India. |
| It is not recognised by Indian law or judicial precedents. | It was recognised in Common Cause vs Union of India as part of the right to die with dignity under Article 21. |
Procedure of Passive Euthanasia in India
The procedure for passive euthanasia in India is based on guidelines laid down by the Common Cause vs Union of India and later simplified by the Supreme Court of India in 2023. It ensures a balance between patient autonomy and medical safeguards.
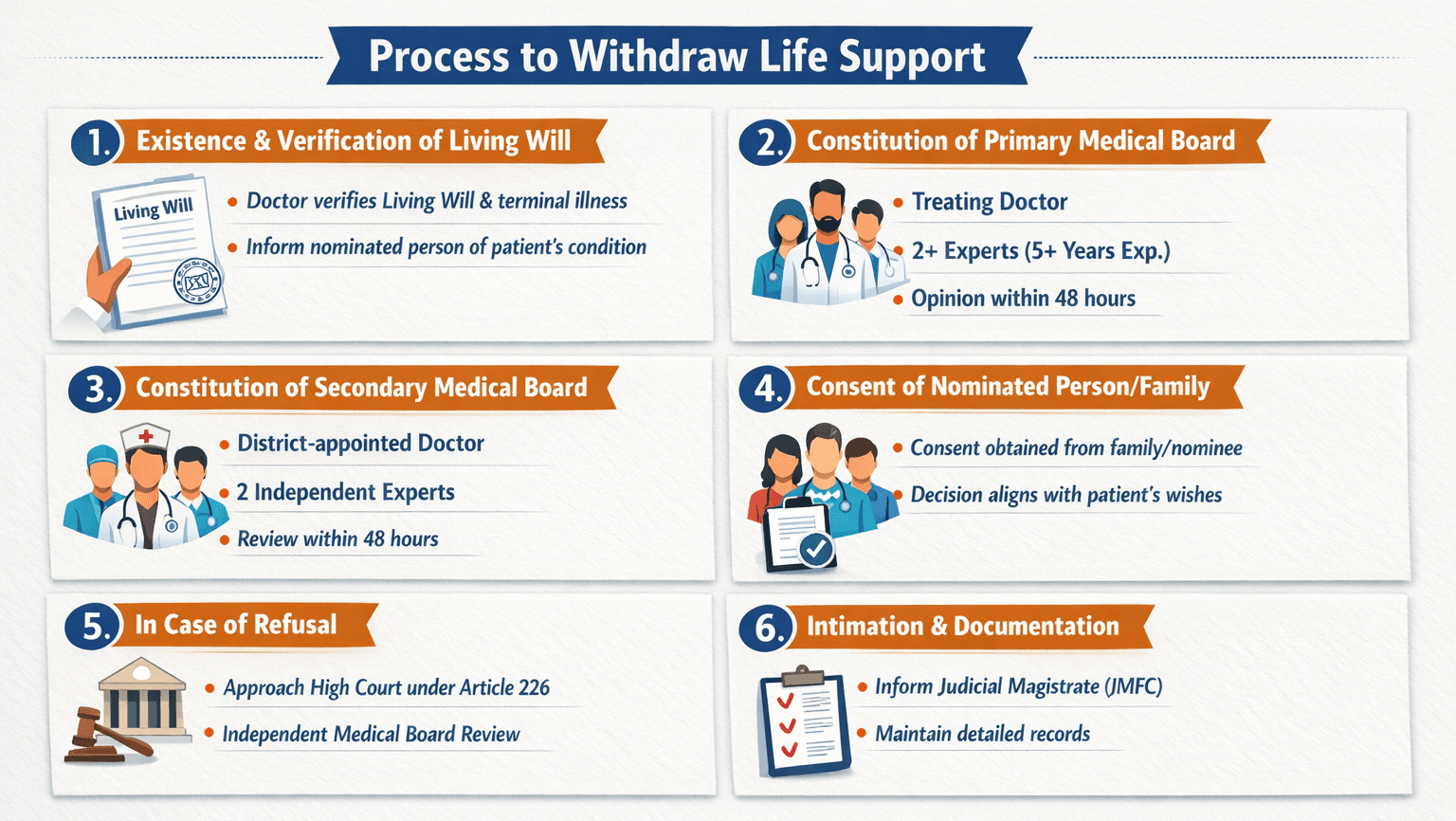
Step-by-Step Process to Withdraw Life Support
1. Existence and Verification of Living Will
- A Living Will allows a person to state in advance their refusal of life-sustaining treatment if they lose decision-making capacity.
- The treating doctor verifies the authenticity of the directive and confirms that the patient is terminally ill with no reasonable chance of recovery.
- The doctor informs the nominated person(s) about the patient’s condition and available medical options.
Simplified 2023 rules: A Living Will can be signed in the presence of two witnesses and attested by a notary or gazetted officer (no need for JMFC approval at this stage).
2. Constitution of Primary Medical Board
The hospital forms a Primary Medical Board, consisting of:
- The treating physician
- At least two subject experts with a minimum of 5 years’ experience
The board examines the patient in the presence of family/guardians and gives its opinion within 48 hours on whether withdrawal of treatment is justified.
3. Constitution of Secondary Medical Board
If the Primary Board approves, a Secondary Medical Board is formed, consisting of:
- One doctor nominated by the District Chief Medical Officer
- Two independent subject experts (not part of the first board)
- This board reviews the case and provides its decision within 48 hours.
4. Consent of Nominated Person/Family
- If the patient is incapable of communicating, consent is obtained from the person(s) named in the Living Will.
- The decision must align with the patient’s expressed wishes, ensuring respect for their autonomy.
5. In Case of Refusal
- If the Secondary Medical Board does not approve withdrawal, the family, nominee, or hospital can approach the High Court under Article 226.
- The Court may constitute an independent medical board and decide in the patient’s best interest.
6. Intimation and Documentation
- The hospital documents the entire process and informs the Judicial Magistrate First Class (JMFC) about the decision.
- Proper records, including consent and medical opinions, are maintained to ensure transparency and legality.
Must read: India's HPV Vaccination Drive: Cervical Cancer - UPSC Notes
UPSC Prelims MCQ on Euthanasia
QUESTION 1
Medium
Indian Polity
With reference to Passive Euthanasia in India, consider the following statements:
- Passive euthanasia is legally permitted under guidelines laid down by the Supreme Court of India.
- Active euthanasia is legal in India under the Bharatiya Nyaya Sanhita.
- Living Will (Advance Directive) has been recognised as valid in India.
Which of the statements given above is/are correct?
Select an option to attempt
Key Judgements on Euthanasia in India
The Indian judiciary has gradually evolved its stance on whether the Right to Life under Article 21 includes the Right to Die, ultimately recognising the idea of a dignified death under strict safeguards.
1. P. Rathinam v. Union of India (1994)
The Supreme Court of India held that the Right to Life includes the Right to Die. It reasoned that just as freedom of speech includes the right not to speak, the right to live could include the right not to live.
2. Gian Kaur v. State of Punjab (1996)
The Court overruled the Rathinam judgment and held that Article 21 protects life and cannot include the right to end one’s life. It stated that suicide is an unnatural extinction of life and not a protected right.
3. Aruna Shanbaug Case (2011)
In this landmark case, the Court allowed passive euthanasia under strict safeguards for the first time. It ruled that withdrawal of life support for an incompetent patient could be permitted, but only with approval from the High Court under Article 226.
The decision also introduced the parens patriae principle, requiring courts to act in the patient’s best interest, and mandated medical board opinions and consultation with relatives.
4. Common Cause vs Union of India (2018, refined in 2023)
A Constitution Bench recognised the Right to Die with Dignity as a part of Article 21. It legalised passive euthanasia and validated Living Wills (Advance Directives).
The Court laid down detailed safeguards, including approval by medical boards, and clarified that withdrawal of treatment must be based on the patient’s best interest. These guidelines were further simplified in 2023.
5. Harish Rana v. Union of India (2026)
The Supreme Court of India authorised passive euthanasia in a real case, marking the first practical application of earlier guidelines. The Court held that Clinically Assisted Nutrition and Hydration (CANH) qualifies as medical treatment and can be withdrawn if it offers no therapeutic benefit.
It emphasised a “dignified exit” and mandated a proper palliative care plan (e.g., at AIIMS) to ensure the patient does not suffer pain.
Arguments For and Against Legalisation of Passive Euthanasia
The legalisation of passive euthanasia in India has sparked an important debate involving constitutional rights, ethical values, and social concerns. While it is supported as a means to ensure dignity in death, it also raises fears of misuse and moral dilemmas.
| Arguments in Favour | Arguments Against |
|---|---|
| Passive euthanasia supports the Right to Die with Dignity, recognised by the Supreme Court of India in Common Cause vs Union of India as part of Article 21. | There is a risk of misuse and coercion, where vulnerable individuals such as the elderly or disabled may be pressured to withdraw life support. |
| It respects patient autonomy by allowing individuals to make decisions about their own medical treatment, including refusal of life support. | India’s weak healthcare and palliative care system may push euthanasia as an easier alternative instead of improving end-of-life care. |
| It helps in protecting human dignity by preventing prolonged suffering or existence in a persistent vegetative or terminal condition. | Diagnostic uncertainty remains a concern, as some patients have shown unexpected recovery despite poor prognosis. |
| It recognises the validity of Living Wills (Advance Directives), ensuring that a person’s medical wishes are respected even when they cannot communicate. | There is strong moral and cultural opposition in India, where many traditions consider life sacred and oppose withdrawal of life support. |
Ethical Aspects of Passive Euthanasia
Passive euthanasia raises complex ethical questions as it involves balancing human dignity, individual autonomy, and the sanctity of life. The debate is not just legal but deeply moral, especially in end-of-life care.
- Autonomy vs Sanctity of Life: While patients have the right to make decisions about their own body (autonomy), many ethical and religious views emphasise that life is sacred and should be preserved at all costs.
- Dignity vs Prolonged Suffering: Passive euthanasia is often justified as a way to ensure a dignified death when medical treatment only prolongs suffering without hope of recovery. However, critics argue that withdrawing life support may still undermine the inherent value of life.
- Best Interest of the Patient: Decisions are often made when the patient cannot communicate. This raises ethical concerns about whether the choice truly reflects the patient’s wishes or the judgement of doctors and family members.
- Role of Doctors: Medical professionals face a moral dilemma between their duty to save lives and the need to reduce suffering. Passive euthanasia challenges traditional medical ethics, particularly the principle of “do no harm.”
Euthanasia Laws in Other Countries
Different countries follow varied legal approaches to euthanasia and assisted dying, balancing individual autonomy, medical ethics, and legal safeguards.
| Country | Legal Status & Key Features |
|---|---|
| Australia | Voluntary Assisted Dying (VAD) is legal across all six states with strict eligibility criteria and safeguards. |
| Belgium | Legal since 2002; expanded in 2014 to allow minors of any age with parental consent and strict medical criteria. |
| Canada | Medical Assistance in Dying (MAiD) legal since 2016; expansion to mental illness postponed till 2027. |
| France | Active euthanasia is illegal; passive euthanasia and deep sedation are allowed under strict conditions. |
| Germany | Assisted suicide is partially permitted after a 2020 court ruling; active euthanasia remains illegal. |
| Japan | No specific law; withdrawal of life support allowed under limited circumstances. |
| Netherlands | Legal since 2002 under strict conditions; extended in 2023 to include children (1–12 years). |
| Switzerland | Assisted suicide is legal if not motivated by selfish interests; active euthanasia is illegal. |
| United Kingdom | Both euthanasia and assisted suicide are illegal, though debates continue. |
| United States | Permitted in several states under “Death with Dignity” laws with strict medical oversight. |
Also see: Amoebic Meningoencephalitis: Brain-Eating Amoeba [UPSC]
UPSC Mains Practice Question on Euthanasia
“The legalisation of passive euthanasia in India reflects a shift from the right to life towards the right to die with dignity.” Discuss in the light of recent judicial developments. (250 words, 15 marks)
Evaluate your Answer within 60 SecondsConclusion
“Dignity is not just how we live, but also how we leave life.”
Passive euthanasia in India reflects this idea by recognising that end-of-life care should be guided by compassion, dignity, and respect for individual choice. As upheld in Common Cause vs Union of India, the focus is not on ending life, but on allowing a natural and dignified death when recovery is no longer possible.
Going forward, the real challenge lies in ensuring strong safeguards, ethical medical practice, and better palliative care, so that dignity in death becomes a reality for all, without risking misuse.
Start your UPSC Preparation 2026/2027 with SuperKalam
SuperKalam is your personal mentor for UPSC preparation, guiding you at every step of the exam journey. Practice, revise, and evaluate– all in one place.
Download the SuperKalam App Now


